Artificial Intelligence Resource Center

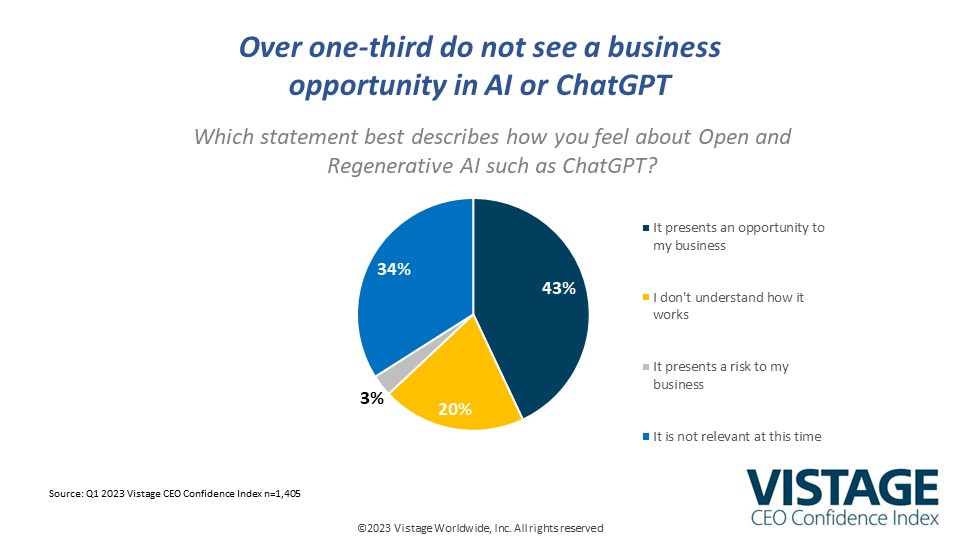
Artificial intelligence has rushed to the forefront of business with the recent emergence of Open and Generative AI platforms such as ChatGPT. CEOs and executives are scrambling to take advantage of this new technology and its potential for disruption. In fact, 43% of CEOs believe it presents an opportunity for their businesses, according to our Q1 2023 CEO Confidence Index survey. But for all the opportunities that abound, there’s also confusion as to how it works, how it can be used, and whether there are risks involving cybersecurity.
To better navigate the complexities surrounding artificial intelligence — from its everyday uses to the rise of machine learning and the future of automation — Vistage has created this resource center to bring you the latest information, thought leadership and best practices surrounding AI. Here’s our latest on the big-picture implications of AI and how it can transform business.
To help with your decision-making, we’ve curated the following:
- Networks & Conversations (including our new AI Network!)
- Webinars & Events
- Expert Speakers
- Trusted Resources by Topic
Network & Conversations
[New] Artificial Intelligence (AI) Network
Join our new AI Network, the go-to place for peers to discuss the thoughtful adoption of AI in business through new policies, technologies, standards and perspectives (password req’d).
Network Conversations
- Looking for Chat GPT Plug-Ins [Artificial Intelligence Network]
- AI for recreating graphics? [Artificial Intelligence Network]
- AI = CoPilot vs Anthropic [Financial Services Network]
- Fathom AI notetaker Zoom problems [Artificial Intelligence Network]
- AI tools recommendations [Artificial Intelligence Network]
- Power of AI and ERP in Manufacturing [Manufacturing Network]
- AI for estimating [Construction Network]
- Creating custom GPT for CPG brand marketing [Artificial Intelligence Network]
- AI prompts/prompting training [Artificial Intelligence Network]
- AI for beginners – seeking tools [Artificial Intelligence Network]
Webinars & Events
How AI Supercharges Your ERP Data | On-demand
Vistage CE member and CEO of WM Synergy, Paul Tedford, shared real-life examples of how SMB manufacturers are leveraging their own internal system data with AI to enhance their business.
Take the First Step Towards Unleashing the Power of AI & ERP in Manufacturing | 30-min On-demand
Vistage CE member and CEO of WM Synergy, Paul Tedford, delivers a teaser of how manufacturers can harness AI to unlock automation and efficiency opportunities.
Artificial intelligence roundtable: Best practices from small businesses | On-demand
Three Vistage members share their experiences with artificial intelligence. They discuss its practical uses, the positive outcomes they’ve seen and the valuable lessons they’ve learned along the way.
AI 101: The basics for business leaders series | 3-Part Series On-demand
AI 101 series for business leaders – a comprehensive three-part journey that will help demystify the ever-evolving world of AI and equip you with the knowledge to harness its potential.
Expert roundtable: Navigating Artificial Intelligence for CEOs | On-demand
A trio of Vistage experts provides a comprehensive breakdown of AI and its different applications for small and midsize businesses. Gain the knowledge to make informed decisions and get buy-in from your team.
Navigating the Future of Business with AI and ChatGPT | On-demand
An expert panel of Vistage speakers breaks down the impact of these emerging technologies on business and how to leverage them for better results.
Expert Speakers
Looking for an expert to work with your company or speak to your group? Click below to learn more about these speakers in the Vistage community (password req’d).
- Brian Burke: Understanding and using ChatGPT to 10x productivity
- Andrew Louder: The Power of AI and ChatGPT: Unleash Productivity and Profits
- Mike Foster: Cybersecurity and Artificial Intelligence: What Key Executives Need to Know
- Dave Nelsen: The Future and How to Prosper in IT
- Ross Hartman: Leveraging AI for Executive Success: Practical Applications and Strategies for Transforming Your Business with Artificial Intelligence
- Tom Young: AI and the Future of Marketing
- Michael Stratta: Moneyball for Business: Using AI and Data Science in Today’s Competitive Environment
- Oliver Buechse: Smart Start Your Digital Transformation
- Severin L. Sorensen: The AI Whisperer: Handbook for Leveraging Conversational Artificial Intelligence and ChatGPT for Business
- David Karandish: Three Key Steps To Get Employees Comfortable With AI In The Workplace
Trusted Resources by Topic
What is AI, and what are its business applications?
Can AI-driven innovation outperform [Vistage]
How businesses can fully harness the power of generative AI [Vistage]
How managers can leverage the productivity promise of generative AI [Vistage]
What Can AI Do For My Company [Vistage Perspectives]
3 ways leaders can start unlocking the benefits of AI [Vistage]
Michael Rogers: 5 questions about AI and the future of business [Vistage]
AI best practices: 3 CEOs share how they are using emerging technologies [Vistage]
Michael Rogers: Why AI security is a priority now [Vistage]
Technology trends for 2024 and beyond [Vistage]
Artificial Intelligence Commission: Preparing for the Future [U.S. Chamber of Commerce]
6 frequently asked questions about artificial intelligence that CEOs need to answer [Vistage]
How AI will unleash an innovation revolution [Vistage]
4 key insights about artificial intelligence from a futurist [Vistage]
CEOs are caught between the ‘fear of missing out’ on AI — and the ‘fear of getting in’ [Forbes]
How To Get Your Team Comfortable With AI: Insights From A Microsoft Executive [Forbes]
What is AI? Learn About Artificial Intelligence [Oracle]
What every CEO should know about generative AI [McKinsey & Company]
A CEO’s 5-Step Process for Navigating Disruptions like ChatGPT [Fast Company]
Artificial intelligence for small and midsize businesses [Vistage]
The rise of artificial intelligence, explained [Vox]
Types of AI
5 AI Trends to Watch in 2023 [Built In]
Types of Artificial Intelligence That You Should Know In 2023 [Forbes]
The 5 Biggest Artificial Intelligence (AI) Trends in 2023 [LinkedIn]
Guidelines and Policies
Three things to know about how the US Congress might regulate AI [MIT Technology Review]
Make Sure Generative AI Policies Cover Intellectual Property [SHRM]
AI Regulation Is Coming [HBR]
AI Regulation in the U.S.: What’s Coming and What Companies Need to Know in 2023 [Law.com]
2023 Will Be The Year of AI Ethics Legislation Acceleration [Forbes]
Security and risks
Generative AI-nxiety [ HBR]
Cybersecurity Trends & Statistics For 2023; What You Need To Know [Forbes]
Addressing the Security Risks of AI [Lawfare Institute]
Artificial Intelligence (AI) for Cybersecurity [IBM]
Sales, Marketing & Customer Service
How to Introduce Your Employees to Artificial Intelligence [Inc.]
Artificial intelligence for small business: 5 lessons from an early adopter [Vistage]
The next frontier of customer engagement: AI-enabled customer service [McKinsey & Company]
Generative AI Will Enhance — Not Erase — Customer Service Jobs [HBR]
Talent
AI Could Drive A Push For Re-Skilling [Forbes]
Pros and Cons of Coaching with AI [Forbes]
Is ChatGPT the Answer to a More Equitable Workplace? [Great Place to Work]
ChatGPT and AI are the next worker recruitment and retention game-changers [CNBC]
2023 HR Technology Trends: Talent Marketplaces, Expanding AI and Optimizing Existing Systems [SHRM]
Related Resources
Category : Technology
Tags: artificial intelligence, emerging technologies, Technology, technology trends affecting business
